Indexing & Abstracting
Full Text
Short CommunicationDOI Number : 10.36811/ijdsc.2019.110003Article Views : 21Article Downloads : 25
Acute hemorrhagic edema of young children: open questions and perspectives
Pietro O. Rinoldi1, Gregorio P. Milani1,2,3, Mario G. Bianchetti1,4, Alessandra Ferrarini1, Gian Paolo Ramelli1, and Sebastiano A. G. Lava5
1Pediatric Institute of Southern Switzerland, Ospedale San Giovanni, Bellinzona, Switzerland
2Pediatric Unit, Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico, Milan, Italy
3Department of Clinical Sciences and Community Health, Università degli Studi di Milano, Milan, Italy
4Università della Svizzera Italiana, Lugano, Switzerland
5Pediatric Cardiology Unit, Department of Pediatrics, Centre Hospitalier Universitaire Vaudois, 1010 Lausanne, Switzerland
*Corresponding Author: Dr. Mario G. Bianchetti, Università della Svizzera Italiana, Via Buffi, 6900 Lugano, Switzerland, Email: mario.bianchetti@usi.ch
Article Information
Aritcle Type: Short Communication
Citation: Pietro O. Rinoldi, Gregorio P. Milani, Mario G. Bianchetti, et al. 2019. Acute hemorrhagic edema of young children: open questions and perspectives. Int J Dermatol Skin Care. 1: 63-67.
Copyright: This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Copyright © 2019; Pietro O. Rinoldi
Publication history:
Received date: 27 June, 2019Accepted date: 16 July, 2019
Published date: 17 July, 2019
Introduction
Childhood vasculitis is a challenging group of conditions that are often multisystem in nature and may require integrated care from multiple pediatric subspecialists, including cardiologists, dermatologists, gastroenterologists, nephrologists, neurologists, and rheumatologists. Apart from Henoch Schönlein syndrome, recently renamed immunoglobulin A vasculitis, and Kawasaki disease, which are reltively common, there are a number of important but comparatively rare vasculitides affecting children [1-4].
Acute hemorrhagic edema of young children [5-8] is a skin limited nongranulomatous leukocytoclastic small-vessel vasculitis, which usually develops in previously healthy subjects after a simple, mostly viral, febrile illness (more rarely after a vaccination). The condition was initially reported in 1913 by Irving Snow in the United States and in 1936 by Mario Del Carril in Argentina [5,6]. The most comprehensive descriptions, however, were made in Germany before the Second World War by Heinrich Finkelstein (1865–1942) and later by Hubert Seidlmayer (1910–1965). A significant description was also made in 1942 by Marcel Lelong (1892-1973) in France [5,6].
Acute hemorrhagic edema has been known with a variety of synonyms: acute hemorrhagic edema of young children (or infancy), cockade (or iris-like) purpura and edema of young children, Henoch–Schönlein syndrome of early childhood, Finkelstein-Seidlmayer syndrome, Finkelstein syndrome and Seidlmayer syndrome [5,6,8].
Open questions
In our opinion, there are at some problems with acute hemorrhagic edema of young children.
• Standardized nomenclature and definition
In everyday clinical practice, the mainstay of the diagnosis is based on symptoms and signs alone (Table 1). The crucial diagnostic clue, is, in our opinion, the acute onset of frightening erythematous annular skin lesions sparing the trunk and a diffuse non-pitting body edema in a well appearing infant, which is often afebrile (Figure 1). Standardized names and definitions are obviously a prerequisite for developing validated classification and diagnostic criteria for cutaneous vasculitis. Regrettably, however, no criteria for the classification of acute hemorrhagic edema of childhood have been included in the recent update on the nomenclature for cutaneous vasculitis [9,10].
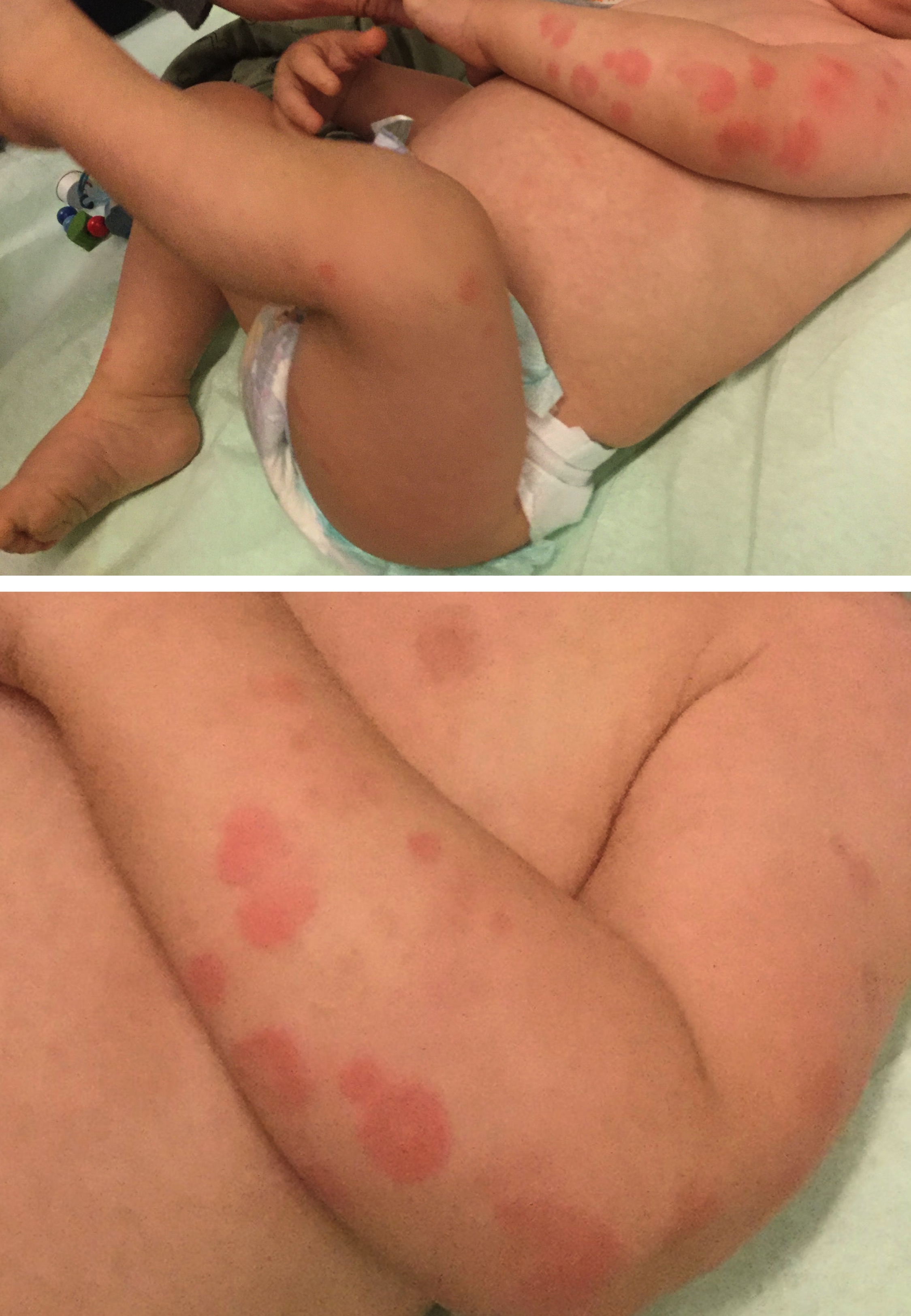
Figure 1: Legend
Seventeen-month-old female presented to the emergency department with a 2-day history of a progressive rash and swelling that started on her lower extremities and rapidly spread to the upper extremities, face and ears. Physical examination revealed an afebrile well-doing infant with multiples erythematous annular lesions sparing the trunk and a diffuse non-pitting painless body edema. No scratching was seen. Laboratory examination revealed normal total blood cell count without leukocytosis, C-reactive protein and urinalysis. The girl had recently been managed by her pediatrician for a common cold. Rash and edema normalized within 5 days. The test for detection of 26 respiratory viruses and Mycoplasma pneumoniae in a nasopharyngreal swab was negative. Consent to the use of the photographs was obtained.
|
Table 1: Currently recommended diagnostic clues for acute hemorrhagic edema of young children. |
|
• Age: ≤24 months • Clinical features: a) non-pitting and often tender edema of the face, auricles, and extremities; b) targetoid lesions over the cheeks, ears, and extremities (with relative sparing of the trunk); c) no scratch marks, no pruritus • Not-ill-appearing infant: normal eye contact with ability to recognize parents or to interact with persons or objects in the environment, absent cyanosis or pallor, absent coldness of the extremities with capillary refill ≤2 seconds in “warm” environment, respiratory rate neither increased nor decreased • Absent articular, abdominal or renal* involvement • Recovery time: ≤2-[3] weeks |
|
*dipstick urinalysis is advised but not compulsory in children with characteristic features and absent articular and abdominal involvement. |
• Unknown prevalence
Acute hemorrhagic edema is considered very uncommon. More importantly, little information is available on its prevalence. We found in the literature four case series publishdd between 2007 and 2016 including apparently unselected pediatric patients with either Henoch-Schönlein or acute hemorrhagic edema: 329 cases with the former and no more than 18 (approximately 5%) cases with the latter condition. These data apparently confirm the low prevalence of the condition. In our opinion, however, acute hemorrhagic edema is likely underrecognized (and underreported). This is mainly due to the fact that the diagnosis of infantile erythema multiforme*, that of unclassified infection-associated skin rash or perhaps also that of atypical Waterhouse-Friderichsen syndrome is usually made in affected patients.
• Presentation - management
The most characteristic presentation and course of acute hemorrhagic edema have been rather well characterized. However, some statements are uncritically handed down from one publication to another without any persuasive proof on the subject. Some examples. A) Many authors state that the condition does not affects subjects more than 24 months of age and consequently discourage the use of the term “acute hemorrhagic edema of young children” and prefer referring to the conditon as “acute hemorrhagic edema of infants”. B) Furthermore, it has been frequently stated the acute hemorrhagic edema is often triggered by a Mycoplasma pneumoniae respiratory disease (likely because this microorganism has been associated with erythema multiforme, a condition resembling, as previously stated, acute hemorrhagic edema). C) Finally, no data support current practice of treatment with antihistamines, corticosteroids, or both. The reasons underlying the mentioned undocumented statements are related to the fact that acute hemorrhagic edema has so far been documented in approximately 300 articles (a large subset of them is not included in the United States National Library of Medicine and in Excerpta Medica Databases) including one to two cases each [5,6].
• Henoch-Schönlein syndrome of early childhood
Acute hemorrhagic edema is often deemed to be the infantile variant of Henoch-Schönlein syndrome. This hypothesis is supported by an Italian report documenting the simultaneous appearance of acute hemorrhagic edema and Henoch-Schönlein syndrome in a brother and a sister. Cases also exist, who have features overlapping between acute haemorrhagic edema and Henoch-Schönlein syndrome. On the other hand, there are sufficient differences to consider acute hemorrhagic edema of young children a separate entity, including the very different skin features, the skin isolated involvement, and the failure to detect depositions of immunoglobulin A in most biopsies. Consequently, Finkelstein– Seidlmayer syndrome and typical Henoch- Schönlein syndrome are presently thought to be clinically separate conditions [5,6].
A coming of age for acute hemorrhagic edema of young children
The evidence from systematic reviews, currently considered as especially reliable, is often used to inform on cause, risk factors, clinical features, prognosis and complications of a disease. Nonetheless, clinical practice based on valid evidence is especially challenging in the field of rather rare diseases such as acute hemorrhagic edema [11]. To overcome at least in part this difficulty, we recently developed the acute hemorrhagic edema bibliographic database AHEBID, which progressively integrates all the original articles on acute hemorrhagic edema published in Dutch, English, French, German, Italian, Portuguese, Spanish and Turkish after the original report by Snow in 1913. For this purpose, we used the Excerpta Medica and US National Library of Medicine databases, Google and especially the medical literature folder on acute hemorrhagic edema started by one of us in the early eighties. The literature will be systematically screened by two members of our group every second month. AHEBID project currently contains bibliographic records on more than 450 individually documented and published cases of acute hemorrhagic edema that have been published since 1970. It also integrates the articles published before 1970, including among others the seminal reports by Snow, by Del Carril, by Finkelstein, by Seidlmayer and by Lelong. The data, which are currently being extracted, are not yet lodged in a publicly accessible archive. It is our hope that they will be used to provide greater insight into the triggers and both the typical and atypical features of acute hemorrhagic edema of childhood. More importantly, we hope that that the results will help developing consensus guidelines relating to diagnosis and management of this skin-limited vasculitis.
References
1. Dillon MJ, Ansell BM. 1995. Vasculitis in children and adolescents. Rheum Dis Clin North Am. 21: 1115-1136. Ref.: https://bit.ly/2XFtREC
2. Dedeoglu F, Sundel RP. 2005. Vasculitis in children. Pediatr Clin North Am. 52: 547- 575. Ref.: https://bit.ly/2JAh9OX
3. Weiss PF. 2012. Pediatric vasculitis. Pediatr Clin North Am. 59: 407-423. Ref.: https://bit.ly/2NWHJpJ
4. Lakdawala N, Fedeles F. 2017. Vasculitis: Kids are not just little people. Clin Dermatol. 35: 530-540. Ref.: https://bit.ly/2ShkmFM
5. Fiore E, Rizzi M, Ragazzi M, et al. 2008. Acute hemorrhagic edema of young children (cockade purpura and edema): a case series and systematic review. J Am Acad Dermatol. 59: 684-695. Ref.: https://bit.ly/2YNYxjz
6. Fiore E, Rizzi M, Simonetti GD, et al. 2011. Acute hemorrhagic edema of young children: a concise narrative review. Eur J Pediatr. 170: 1507-1511. Ref.: https://bit.ly/2LlhJlK
7. Ting TV. 2014. Diagnosis and management of cutaneous vasculitis in children. Pediatr Clin North Am. 61: 321-346. Ref.: https://bit.ly/2XJ9hU2
8. Lava SAG, Milani GP, Fossali EF, et al. 2017. Cutaneous manifestations of smallvessel leukocytoclastic vasculitides in childhood. Clin Rev Allergy Immunol. 53: 439-451. Ref.: https://bit.ly/2GdHj7T
9. Sunderkötter CH, Zelger B, Chen KR, et al. 2018. Nomenclature of Cutaneous Vasculitis: Dermatologic Addendum to the 2012 Revised International Chapel Hill Consensus Conference Nomenclature of Vasculitides. Arthritis Rheumatol. 70: 171-184. Ref.: https://bit.ly/2JzaJPY
10. Caproni M, Verdelli A. 2019. An update on the nomenclature for cutaneous vasculitis. Curr Opin Rheumatol. 31: 46-52. Ref.: https://bit.ly/30xPLXf
11. Bianchetti MG, Zufferey-Caiata M, Milani GP, et al. 2015. Rare disorders: the role of accurate case-based research, inquiries and qualitative research. J Rare Disord Diagn Ther. 1: 7.




















