Indexing & Abstracting
Full Text
Case ReportDOI Number : 10.36811/ojprm.2020.110007Article Views : 16Article Downloads : 20
Giant Mediastinal Ganglioneuroma in a Female Child
Yasser A El Sayed1*, Moh Fathy2, Mohammad Aleem3, Alaa Eisa4, Ashraf Enait5, Kerolos Emad6, Bothinah A Al Haseeb7 and Mona Atef8
1Prof. of Thoracic Surgery at the Medical Military Academy, Egypt
2Ass.Prof. of Neurosurgery, Al Azhar University, Egypt
3Cardiothoracic Surgery specialist, Egypt
4Resident of Cardiothoracic Surgery, Egypt
5Prof. of Interventional Radiology, Egypt
6Consultant Anesthesia, Egypt
7Consultants of Pediatrics, Abbasia Pulmonary Hospital, Egypt
8Consultants of Pediatrics, Abbasia Pulmonary Hospital, Egypt
*Corresponding Author: Dr. Yasser A El Sayed, Prof. of Thoracic Surgery at the Military Medical Academy, Cairo, Egypt, Email: Yasser.elsaid33@yahoo.com
Article Information
Aritcle Type: Case Report
Citation: Yasser A El Sayed, Moh Fathy, Mohammad Aleem, et al. 2020. Giant Mediastinal Ganglioneuroma in a Female Child. Open J Pulm Respir Med. 2: 07-10.
Copyright: This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Copyright © 2020; Yasser A El Sayed
Publication history:
Received date: 27 January, 2020Accepted date: 06 February, 2020
Published date: 07 February, 2020
Abstract
We report an eight year female patient admitted to the department of pediatrics at Abbasia Pulmonary Hospital at Cairo, Egypt. The child was complaining of pain on the right lower chest and upper abdome. On evaluation by CT of the chest, there was a huge posterior mediastinal mass occupying more than three quarters of the right hemithorax. Preoperative histopathology using CT guided needle biopsy revealed ganglioneuroma. The tumor was resected completely via right standard postero-lateral thoracotomy without complications. Postoperative histopathology confirmed the diagnosis of ganglioneuroma.
Keywords: Ganglioneuroma; Posterior mediastinum; Pediatrics
Introduction
Ganglioneuromas are rare benign neurogenic tumors which arises from neural crest cells that represents the final maturation stag of neuroblasts [1]. The incidence of ganglioneuroma was reported to be 1 in 1,000,000 and thought to develop de novo rather than by maturation of existing neuroblastoma [2]. There are no known risk factors, however the tumors may be associated genetic problems , such as neurofibromatosis type 1 [3]. Ganglioneuromas are commonly classified as pediatric mediastinal tumors occurring in females more than males with a ratio about 3:1 [4]. Most of the cases are asymptomatic and usually discovered accidentally. The most common sites of ganglioneuromas are the posterior mediastinum and retroperitoneum (37.5% each) [5]. Surgical resection of mediastinal ganglioneuroma is the treatment of choice [6]. The aim of this report is to present a case of ganglioneuroma in an eight years old female, to show its mode of presentations, different preoperative tools used for the diagnosis and the standard line of treatment in such cases which is complete surgical resection.
Case Report
Female child 8-years old presented with her mother to the outpatient clinic of the pediatric department at Abbasis Pulmonary Hospital, Cairo governorate, Egypt. The child was complaining of repeated right sided chest pain. The pain started 4 months before presentation to our hospital, the pain is sharp in character and mild in intensity. The pain was affecting the lower part of the right chest, and sometimes referred to the upper abdomen. The pain is on and off in character and each time lasts about one minute or two. The pain had no aggravating or relieving factors. There was no history fever, weight loss no GIT symptoms or other respiratory symptoms. The history of the pregnancy given by her mother was normal with vaginal delivery. Also, all the child developmental milestones were normal. Family history and consanguinity were negative. A plain chest X-ray P-A view was done in the outpatient clinic that revealed a huge well circumscribed, radio opaque, homogenous posterior mediastinal mass (Figure 1). So, the child was admitted to the pediatric department for further evaluation.
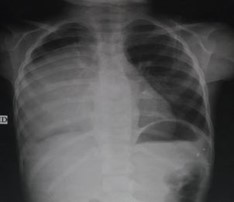
Figure 1: Chest X-ray P-A view showing.
General examination of the child was unremarkable. Chest examination revealed decreased air entry on the right back of the chest with scattered rales. All laboratory investigations were within normal level. CT scan of the chest was done (Figure 2&3) and revealed a giant, non-enhancing about 20 X 23 cm well-defined, more or less rounded mass which is homogenous and non-enhancing. The mass was located on the right hemithorax in the posterior mediastinum. The mass was abutting the thoracic vertebrae in the paravertebral gutter.
Giant opacity occupying most of the right hemithorax.

Figure 2: CT chest mediastinal window.
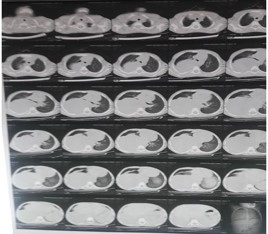
Figure 3: CT chest pulmonary window.
CT guided needle biopsy was taken and histopathology report revealed a ganglioneuroma. After histopatological diagnosis, the patient was referred to the Thoracic surgery department at our hospital for surgery. Surgical resection of the tumor was performed by a team of thoracic and neurosurgery via right slandered postero-lateral thoracotomy in the fifth space. During surgery the tumor was found to be well encapsulated with firm consistency, well circumscribed not invading any nearby structures. Due to the huge size of the tumor, it was resected in two pieces (Figure 4). During operation there was considerable bleeding, so interaoperative embolization of the feeding vessels that stopped the bleeding. The weight of the tumor was 830 gm (Figure 4). Postoerative histopathology confirmed that the tumor was benign ganglioneuroma. The patient had uneventful postoperative course and was discharged from the hospital after 10 days in good condition for regular follow up.
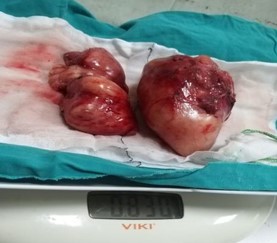
Figure 4: Ganglioneuroma after surgery (weight 830 gm).
Discussion
Ganglioneuroma are rare benign tumors of the autonomic nerve fibers arising from the neural crest sympathogonia. Ganglioneuromas are fully differentiated neuronal tumors that do not contain immature elements. They are typically well encapsulated tumors with a fibrous capsule that arise in the posterior mediastinum [7]. Our case showed a well encapsulated tumor during surgery. Ganglioneuromas occur most commonly in young patients, however they may be found in adult life. They represent the most common tumor arising in the posterior mediastinum in pediatric age group [8]. Our case was a child of 8 years old with a posterior mediastinal ganglioneuroma. Ganglioneuromas are mostly asymptomatic and are known as pediatric intrathoracic incidentoma. They are discovered when the patient is assessed for another disease [9]. Symptoms of the tumor depends on its site and compression effect on the adjacent structures. So, symptoms of mediastinal may include shortness of breath, chest pain or Horner’s syndrome if it compressing the sympathetic ganglia. Retroperitoneal ganglioneuroma may cause abdominal pain and bloating. Compression of the spinal cord by ganglioneuroma may cause motor or sensory loss in the legs, arms or both or spinal deformity [10]. Such tumors may produce certain hormones which can cause diarrhea, enlarged clitoris in women, high blood pressure or sweating [11]. Our case was a posterior mediastinal tumor that y. Radiological studies are very useful tools in suggesting the diagnosis of posterior medistinal ganglioneuroma. Plain X-ray postero-anterior and lateral views show the posterior mediastinal mass well delineated mass that may cause rib spreading and foraminal erosin. CT scan of the chest shows well circumscribed mass which are iso to hypoattenuating to muscle. The tumor may show calcifications in 20% of tumors. The calcifications are typically fine and speckled but may be coarse. MRI also is a useful radiologic modality in diagnosis of mediastinal ganglioneuroma. Mediastinal ganglioneuroma on imaging should be differentiated from cystic teratoma, neurilemmoma, lymphangioma cysticum or bronchocele [12]. The standard treatment of mediastinal ganglioneuroma is surgical excision especially when there are symptoms of compression, marked increase in size or encroaching on the vertebral foramina [13].
Conclusion
From this case presentation we concluded that mediastinal ganglioneuroma is a rare neurogenic tumor that may be asymptomatic or produce vague symptoms in spite of having a huge size. Mediastinal ganglioneuroma can be diagnosed histopathological preoperatively by using CT guided needle biopsy. Surgical resection is mandatory to relieve symptoms and avoid the extremely rare possibility of transformation to malignant form.
References
1. Khan HA, Khan FW, Fatimi SH. et al. 2017. Giant Ganglioneuroma in a 5-Year Child. J of the college of Physicians and Surgeons Pakistan; 27: 16-17. Ref.: https://www.ncbi.nlm.nih.gov/pubmed/28302232
2. Shetty PK, Shetty PK. 2011. Ganglioneuroma always a histopathological diagnosis. Online J Health Allied. 9: 4. Ref.: https://bit.ly/2UpQ4nj
3. El Hammoumi M, Arsalane A, Kabiri H. 2015. Posterior mediastinal gangioneuroma. Arch Bronconeumol. 51: 50-51. Ref.: https://bit.ly/374Adxn
4. Sanal M, Meister B, Kerczy A, et al. 2005. Intrathoracic ganglioneuroma and ganglioneuroblastoma: Report of four cases. European Surger. 37: 317-320. Ref.: https://bit.ly/2UsOW27
5. Geoerger B, Harms D, Grebe J, et al. 2001. Metabolic activity and clinical features of primary ganglioneuromas. 15: 1905-1913. Ref.: https://bit.ly/2v1jmhB
6. Cardillo G, Carleo F, Khalil MW, et al. 2008. Surgical treatment of benign tumors of the mediastinum: a single institution report. Eur Cardiothorac. 34: 1210-1214. Ref.: https://bit.ly/2UqX2Zp
7. Tansel T, Onursal E, Davioalu E, et al. 2006. Childhood mediastinal masses in infants and children. The Turkish J Pediatr. 48: 8-12. Ref.: https://bit.ly/2GUnNNJ
8. Hayat J, Ahmed R, Alizai S, et al. 2011. Giant gamglioneuromas of the posterior mediastinum. Interactive Cardiovascualr and Thoracic Surgery. 13: 344-345. Ref.: https://www.ncbi.nlm.nih.gov/pubmed/21693453
9. Shukla RH, Mukhopadhyay B, Mukhopadhyay M, et al. 2013. Mediastinal gangioneuroma: An incidentoma of childhood. Indian J Med Paediatri Oncol. 34: 130-131. Ref.: https://www.ncbi.nlm.nih.gov/pubmed/24049306
10. Spinelli C, Rossi L, Barbetta A, et al. 2015. Incidental ganglioneuromas: a presentation of 14 surgical cases and literature review. J Endocrinol Invest. 38: 547-554. Ref.: https://www.ncbi.nlm.nih.gov/pubmed/25501841
11. Reeder LB. 2000. Neurogenic tumors of the mediastinum. Semin Thoracic Cardiovasc Surg. 12: 261-267. Ref.: https://bit.ly/380pHbA
12. Pavlus JD, Carter BW, Marc D, et al. 2016. Imaging of thoracic neurogenic tumors. Am J Roentgenology. 207: 552-561. Ref.: https://bit.ly/2Ux0rWF
13. Fraga JC, Aydogdu B, Aufieri R, et al. 2010. Surgical treatment of pediatric mediastinal neurogenic tumors. Ann Thorac Surg. 90: 413-418. Ref.: https://bit.ly/2UqZjDV




















