Indexing & Abstracting
Full Text
Research ArticleDOI Number : 10.36811/osjs.2019.110005Article Views : 11Article Downloads : 23
Slipped cervical disc: Treatment by means of, all in one
Iñaki Arrotegui
Hospital General Universitario de Valencia, Dept. of Neurosurgery, Spain
*Corresponding author: Dr. Iñaki Arrotegui, Consultan Neurosurgeon. MD. Ph. D, Hospital General Universitario de Valencia, Dept. of Neurosurgery, Avda Tres Cruces S/n .46014-Valencia-Spain, Email: athbio@yahoo.es
Article Information
Aritcle Type: Research Article
Citation: Iñaki Arrotegui. 2019. Slipped cervical disc: Treatment by means of, all in one. Open Sci J Surg. 1: 34-40.
Copyright: This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Copyright © 2019; Iñaki Arrotegui
Publication history:
Received date: 09 April, 2019Accepted date: 08 May, 2019
Published date: 09 May, 2019
Concept
Slipped disc is the exit of the nucleus pulposus material through the broken fibrous annulus.
Epidemiology
Along with lumbar disc, cervical disc is one of the most frequent neurosurgical diseases today, probably due to the new habits of modern, more sedentary civilization. The loss of muscle component weakens the complex structure of the spine. Added to this is the attitude maintained, in our usual work position, of the sitting position, inclined slightly forward and with the head bent, which causes an even greater load to be placed on the intervertebral discs than if we are in an upright position. And, to top it off, in an extemporaneous and irregular way, we submit an unusual effort to the column (exercises or sports not well controlled, efforts at work or at home, etc.).
Physiology
This causes cracks or breaks in the different layers of the fibrous annulus. They are episodes of pain in the neck or acute cervicalgia, which remit spontaneously with certain rest and adequate medical treatment. These breaks are made much more frequently backwards and to one of the sides, since it is the weakest area of the fibrous annulus. But when the last layer is broken, the nucleus pulposus mass comes out of its place, finding in its way one of the nerve roots, which is crushed or compressed against the bony walls that form the hole of conjunction. This will cause a painful picture more intense and extensive, which runs or radiates to one of the upper extremities, reaching even the fingers of the hand. It is called cervicobrachial.
To understand the clinical possibilities that may arise in the process of a cervical herniated disc you must take into account several factors:
1. The fibrous ring is very innervated by painful nerve endings. Hence, its rupture produces the picture of cervicalgia, with pain centered in the midline of the neck.
2. The nerve roots have three types of fibers: painful, sensitive and motor. These fibers are extensions of the neurons that are located in the marrow. Like electric cables, these fibers are covered by special cells that isolate them, thanks to a fatty substance they contain called myelin. The painful fibers are those that have less coating and the motor fibers that have a layer of thicker myelin. But this myelin, apart from having an insulating function, also has a mechanical protection mission. Hence, when a nerve is compressed, depending on the energy or force that is exerted, at first it hurts, then it begins to have alterations in sensitivity and, in the end, loss of strength.
3. The cervical intervertebral disc will be subjected to a continuous effort for the mobility of the head. This differentiates it with the lumbar intervertebral disc that is going to be subjected to a greater load than movement. This greater mobility leads to a process of wear or degeneration of the joint between the vertebrae: vertebral arthrosis. As in all osteoarthritis, the bone of the joints grows (what is called osteophytes are formed). This growth will occupy and close the space of the vertebral canal and that of the conjunction holes.
4. This process of osteoarthritis or cervical spondylosis will affect, in most cases, several intervertebral discs (most frequently, at the C5-C6 and C6-C7 levels).
5. Therefore, the compression of the nerve roots or the medulla, at the level of the cervical spine, will be produced more by a bone component (osteophytes) than by the herniated nucleus pulposus. This makes some doctors sometimes make the distinction between hard disk (osteophyte) and soft disk (true slipped disc)
6. Rarely, the exit of disc material is massive and penetrates the canal, compressing the cord and causing a serious neurological deficit, with loss of strength in the upper and lower extremities (tetra paresis or tetraplegia).
Types
There is confusion about the types or degrees of herniated disc. Especially today when, thanks to Magnetic Resonance, we can see with great precision the anatomy of this region. In order to clarify the concepts, several types or degrees could be defined.
Disk protrusion
The nucleus pulposus has not yet left the fibrous annulus. But this one, having fewer intact layers, is weaker and yields in its structure, allowing the nucleus pulposus to push it and make a certain imprint on the vertebral canal, surpassing the line of the adjacent vertebral bodies. It is not, therefore, a true herniated disc, but the beginning of the process.
Slipped disc
It is the exit of the nucleus pulposus material from the limits of the fibrous annulus. Although the material is still contained by a very strong fibrous structure.Forms of disc involvementIn the herniated disc, the imprint of the nucleus pulposus within the vertebral canal is greater, as well as the risk of increasing the minimum effort.
Disk extrusion
The exit of the disc material is so violent that it even breaks the posterior common vertebral ligament and there are free fragments in the vertebral canal.
Osteophytosis
As we have already mentioned, in the cervical spine, the continuous process of wear of the intervertebral joint leads to a situation of osteoarthritis with an increase in the bone component at the joint limits (osteophyte or hard disk). So, the root or spinal compression will have a greater bone component than nucleus pulposus herniated.
Clinic
There are several types of discomforts or clinical symptoms, which can be isolated or overlapping.
We will differentiate:
Cervicalgia: The characteristic clinical picture consists of episodes of pain in the neck, occasion of some type of effort or maintenance of a stale posture. In each new episode, the pain takes more days to give in and the episodes are repeated with shorter time intervals.
The person can get to adopt an antalgic posture (torticollis), by muscle contraction to prevent the pain from increasing.
Cervicobrachialgia
After an effort or apparently banal, the person has a very intense pain that runs to one of the arms. The pain increases with any movement, especially when stretching the arm or coughing or sneezing, reaching even the fingers of the hand. You can feel an area as if asleep, cramped or with strange or annoying sensations when touched, which corresponds to the fringe that hurts. In severe cases, the person will also notice loss of strength or ability in the hand, with inability to catch things.
Myelopathy
The previous episodes usually occur in young or middle-aged people. In older people, the clinical picture of myelopathy can be overlapped or isolated. It is usually due more to the presence of osteophytes than to a pure herniated disc. These osteophytes, as they grow or increase in size, end up causing a narrowing of the lumen of the spinal canal (channel stenosis) at the level of one or more vertebral segments [7-9]. Cervical myelopathy consists of an involvement of the spinal cord by chronic or sustained compression of said osteophytes directly on the marrow or on the small vessels that supply blood to the marrow. It is a very slowly progressive clinical picture of difficulty moving the upper limbs and later gait disorders.
Vertebro-basilar insufficiency
It is a worse picture, consisting of episodes of dizziness and feeling of instability. The cause is the involvement of the vertebral arteries as it passes through the cervical spine, due to the growth of these osteophytes, which come to make an imprint on these arteries and decrease their normal caliber. This causes a difficulty in irrigating the areas already mentioned of the brain, spontaneously or with the extreme movements of the neck. The doctor, apart from obtaining the clinical data that allow him to discern between the different clinical pictures, as well as their possible causes, when exploring the patient will appreciate the degree of compression of the nerve root by the intervertebral disc and if any type is added of sensitive affectation and, above all, motor. It will try to delimit the level of the herniated disc and rule out other diagnostic possibilities. In case of myelopathy, the exploration allows measuring the severity of spinal cord involvement. In cases of vertebra-basilar insufficiency, it is the specialist in otorhinolaryngology who has the best means to objectify the affectation and rule out other pathologies that may cause dizziness or dizziness.
There is a very important clinical fact to review. It is a clinical situation consisting of significant pain, but that relatively abruptly disappears, accompanied by significant loss of strength in the hand. This indicates an even greater herniation, which has produced a serious motor impairment, although it has stopped hurting because the mechanical compression of the nerve root has severed the painful conduction. This situation is serious, because we must proceed quickly and agile to a correct diagnosis and possible surgical intervention with an urgent nature, in 24-48 hours, if we want to recover the strength of the hand.
Diagnosis
According to the clinical history and examination, the neurosurgeon will prescribe a series of tests to confirm the diagnosis of herniated disc, the level affected and visualize a possible pathology added: osteoarthritis, vertebral instability.
These tests are, fundamentally:
1. X-ray of the cervical spine, in antero-posterior, lateral and oblique position. It is intended to see the correct or not alignment of the spine, the shape of the vertebral bodies and the spaces between them, as well as the characteristics of the conjunction holes.
In these radiographs there are many indirect signs that enrich the knowledge of the problem that the patient has and that complement the study with Magnetic Resonance.
2. Dynamic radiography of the cervical spine, in the position of flexion and extension of the neck. It is intended to know if there is instability between the vertebrae, which could explain the origin of the herniated disc.
3. Magnetic Resonance: It is the test of choice today. It allows us to clearly see the morphology and relationship of the intervertebral disc with the neighboring anatomical components.
The radiological diagnosis must be read carefully and know how to interpret it. The radiologist who describes the injuries usually makes an exhaustive list of the observed pathology. This, on multiple occasions, leads the patient who reads the reports to understand that he has several herniated discs. But, as a rule, the episode of pain is caused only by one of the altered discs. The others may be in different stages, more or less advanced arthritic degeneration, although of less intensity than the disk that causes the pain.
4. Cat scan or cervical scanner: At the level of the cervical spine, this test has hardly any diagnostic capacity, from the surgical point of view. Bone artifacts are large and it is difficult to obtain clear images of herniated discs.
However, it may be useful as a complement to MRI to better assess the existence of hard disk (osteophyte) and / or soft disk.
5. Electromyogram: It is a simple, although annoying, test that differentiates the affected nerve root, through the study of nerve conduction to the muscles. It is used in patients with a cervical spine in which several discs are already affected and in the Magnetic Resonance image we cannot clearly differentiate which disc is responsible for the clinic that the patient has. Other reasons for its prescription may be the need to objectify a motor impairment or, on the contrary, rule out the existence of a nerve root lesion and, therefore, the need for surgical treatment.
Treatment
When faced with cervicalgia or cervicobrachial, either the first time it presents or another relapsing episode, the first step is to adopt measures that aim to achieve three objectives: to reduce pain, avoid further nerve damage and, if possible, allow nature to solve the problem and obtain healing through conservative means, without surgical intervention. One should only think of a surgical intervention, as a first step, if the condition is accompanied by loss of strength, as we have already mentioned previously. It is advisable, in the first place, relative rest of the cervical spine, to avoid efforts and above all not to maintain the postures of flexion of the neck that would accentuate the herniated disc. In this sense, placement during acute episodes of a cervical collar facilitates rest and avoids performing incorrect movements inadvertently. The medical treatment is based on three types of well-differentiated drugs: analgesics (to reduce pain), anti-inflammatory (to promote recovery of the nerve root of the mechanical trauma of the herniated disc) and muscle relaxants (to cut vicious circles of pain- muscular contracture-pain).
The help of rehabilitation teams, with their massage techniques, magnetic therapy, ultrasound, etc., can make this acute stage shorter. As a result of an episode of cervicalgia or cervicobrachial, it is very important to change the patterns of behavior in daily life, to take care of the spine and prevent the appearance of new episodes. In this sense, advice and control by a rehabilitating medical team is very important Surgical treatment is more clearly defined at the present time than the one we saw in the previous chapter of lumbar disc herniation. Although later we will see it more extensively, in a summarized way the following cases can be presented:
1. Herniated disc and/or osteophyte in one or two intervertebral spaces, with a clinical manifestation of radicular pain or spinal cord involvement. In these cases, microdiscectomy is performed and the superior and inferior vertebrae are fixed or arthrodial to the excised disc.
2. Elderly people and canal stenosis due to marked cervical spondylosis and osteophytes at multiple levels. In these cases, an intervention can be proposed that decompresses the vertebral canal by removing the posterior arches: laminectomy. We will see this in a chapter later.
Cervical Microdiscectomy
The surgical technique consists essentially in the excision of the already damaged intervertebral disc and filling in the remaining space by means of a graft that fixes, one or arthrodesis the superior and inferior vertebrae. But at the cervical level, this technique is very different from the one used in the lower back. These differences are, following the steps of the surgery:
1. Way of approaching: It is done by the anterior and lateral part of the neck (right side from C5-C6 upwards and in left side at level C6-C7).
The anatomical planes of the neck are dissected and a special separator is placed, which carefully removes the esophagus and trachea, leaving a path or free space perpendicular to the intervertebral disc to be intervened.
Previous approach
The surgeon, during the intervention, uses radiological controls, using a portable X-ray machine (image amplifier), so that at any time you want to visualize the surgical maneuvers that are being performed.
2. Microdiscectomy: With the help of a surgical microscope and a highly sophisticated motor, the surgeon maintains correct control in this delicate maneuver. The microscope allows an expanded view of the surgical field and much better illumination than with naked eye techniques. With the engine, thanks to its high speed of rotation (100,000 revolutions / min,) and its specially designed burs, it is possible to go filing the bone with great safety. The disc is removed in its entirety and a small lamina of the vertebral surfaces, until discovering the anterior face of the dura mater that covers the spinal cord. All fragments of the disc or osteophyte that may be compressing the nerve roots or the dura itself are removed.
3. Arthrodesis: Next, a small incision is made at the level of the edge of the hip, to obtain a small fragment of bone that is carved with the motor and adjusts to the size of the space that has remained between the vertebrae. This bone fragment is interposed between the vertebrae and, to facilitate fusion and stability during the period required for osteosynthesis, the procedure is ensured by placing a plate with screws that are fixed on both vertebrae. This plate and its screws are made of titanium, not interfering in the neuroimaging tests that are needed in postsurgical controls. Actually, the permanence of this plaque is necessary only about 3 months, in which the bone graft has fused both vertebrae; but, since it usually does not cause any discomfort, a new intervention is not performed to remove it.
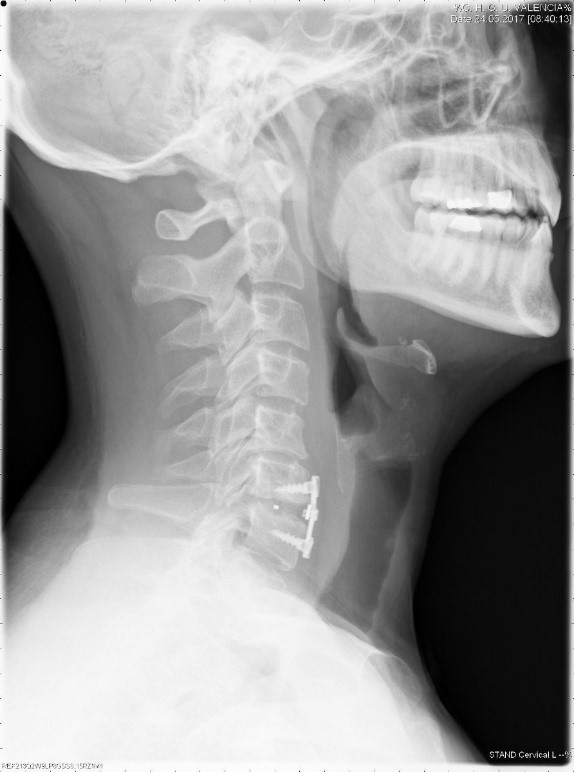
In order to avoid this second incision at the level of the hip, another type of materials to be implanted is proposed. These may be of biological type such as bovine bone, bone substitutes such as hydroxyapatite or ceramic or metallic materials (titanium) in the form of boxes or threaded screws in which bone or bone substitutes are placed. The selection of the implant will depend on the experience of the surgeon and the will of the patient, once the pros and cons of each type of material to be used is known. We present a case of a patient operated on a herniated disc that after the surgery of the disc is placed a plate that determines a saving in the surgical time and allows a fusion of the affected level and a maintenance of the cervical physiological lordosis. (Figure 1 and 2). At the level of the cervical spine, implants that are capable of replacing the intervertebral disc with another system that allows mobility rather than fusion are being attempted. Likewise, techniques for percutaneous approach to the intervertebral disc and the introduction of substances such as chymopapain or ozone have been tried, without having demonstrated a more valid result than the previously described technique.
Figure 1: lateral View all in One.

Figure 2: P_A View all in one.
Discussion
The cervical spine is the most complex and mobile joint system in the body. The degree of structural and functional differentiation of the cervical spine is extraordinary, but the balance of its functionality is constantly threatened, even under physiological conditions. In the last 50 years, various techniques of anterior cervical approach have been developed to treat a wide variety of pathologies. This approach provides access to the dura mater, the nerve roots, the vertebral arteries, and provides considerable flexibility in the access and removal of lesions, as well as the stabilization of the cervical spine. The root and anterior compression of the Spinal cord are the most common indications of the anterior cervical approach. Pathologies such as cervical trauma, acute disc herniation, cervical spondylosis, ossification of the posterior longitudinal ligament, neoplastic processes or infections are some of the pathologies that can be successfully treated by this technique. It is difficult nowadays, and in spite of the many published works to choose which is between the different methods of fixation or non-cervical fixation, the best.
Dr. Leroy Abbot was the first to suggest the previous cervical approach in 1952 while he was a visiting professor in the service of Drs. Bailey and Baddeley [1]. This approach was later used and described by these authors in 19587[2]. In 1958 Robinson and Smith [3] introduced to the technique, the use of the graft. Bone to promote bone fusion during anterior cervical reconstruction. Cloward [4] also followed his technique, and introduced the cylindrical bone graft for anterior cervical fusion. The greatest advance that followed was with the cervical instrumentation initiated by Orozco and Llovet in 1970[5] Cervical fixation technology has developed rapidly in the last three decades [6].
The technical improvements in cervical instrumentation are often the result of innovations that have occurred in relation to complications arising with the previous methods [7]. Although anterior discectomy it is an effective and generally safe measure, it can be associated with a series of complications that may be important due to the related vascular, respiratory, neurological and digestive structures [8,9]. Even though it is considered a safe and simple technique, it is one of the procedures that most commonly receives legal complaints [10].
Conclusions
Surgery of the anterior cervical spine is a simple technique and a surgically safe procedure with a low number of complications. There have been many procedures used to fix the cervical spine, with more than 40 years of experience, and it remains to be defined which is the best. Most of the work done is based on studies from a single institution. It would require more multicenter and prospective cohort studies to compare clinical, radiological, and the presence of complications.
References
- Wang JC, Liang FG, Qu DB, et al. 2005. Risk factors analysis of early complications following anterior spine surgery in 258 cases of cervical spondylitis myelopathy. 25: 450-453. [Ref.]
- Bailey RW, Badley CE. 1960. Stabilization of the cervical spine by anterior fusion. Am J Orthop. 42: 565-594. [Ref.]
- Smith GW, Robinson RA. 1958. The treatment of certain cervical-spine disorders by anterior removal of the intervertebral disc and interbody fusion. J Bone Joint Surg Br (Am). 40: 607-624. [Ref.]
- Cloward RB. 1958. The anterior approach for removal of ruptured cervical disc. J Neurosurg. 15: 602-616. [Ref.]
- Orozco-Declos R, Llovet-Tapies J. 1970. Osteosintesis en las fracturas del raquis cervical: nota técnica. Revista de Ortopedia y Traumatología. 14: 285-288. [Ref.]
- Lunsford LD, Bissonette DJ, Zorub DS. 1980. Anterior surgery for cervical disc disease. Part 2: treatment of cervical spondylotic myelopathy in 32 cases. J. Neurosurg. 53: 12-19. [Ref.]
- Nohra G, Abi-Lahoud G, Jabbour P, et al. 2003. Anterior cervical discectomy with or without bone graft placement in the treatment of cervical radiculopathy. Long-term results. Neurochirurgie. 571-578. [Ref.]
- Nirala AP, Husain M, Vatsal DK. 2004. A retrospective study of multiple interbody grafting and long segment strut grafting following multilevel anterior cervical decompression. Br J Neurosurg. 18: 227-232. [Ref.]
- Omeis I, DeMattia JA, Hillard VH, et al. 2004. History of instrumentation for stabilization of the subaxial cervical spine. Neurosurg Focus. 16: 1-20. [Ref.]
- Samartzis D, Shen FH, Lyon C, et al. 2004. Does rigid instrumentation increase the fusion rate in one-level anterior cervical discectomy and fusion? Spine J. 4: 636-643. [Ref.]




















